Peter Hames, a business development exec working at a karaoke startup in London, wasn't the first insomniac sufferer who tried to convince Professor Colin Espie, a leading sleep disorders expert, to turn his book on Cognitive Behavioral Therapy into
29 min. Read
5.12.23
The Big Health Report
In this article:
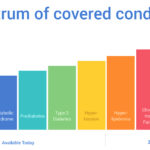
Big Health is a digital therapeutics company at an interesting inflection point: Should it pursue FDA clearance and a prescription pathway? E&O dug into this question and many others in this 7,500-word report. Read on for Big Health’s annual revenues, number of patients treated, pricing, performance guarantee, and much, much more.
×
![]()